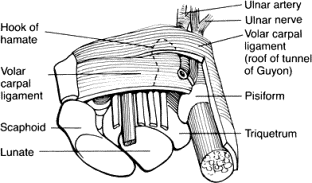
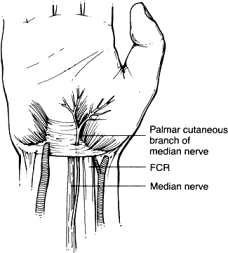
Carpal tunnel syndrome is the most common entrapment neuropathy of the upper extremity. The carpal tunnel is a fibro-osseous canal bound volarly by the transverse carpal ligament; the floor and walls are formed by the carpal bones. The transverse carpal ligament attaches radially to the scaphoid and trapezium and ulnarly to the pisiform and hamate. The flexor pollicis longus, flexor digitorum profundus, and flexor digitorum superficialis tendons traverse the carpal tunnel along with the median nerve. Before entering the carpal tunnel, the median nerve gives off the palmar cutaneous branch, which passes superficial to the transverse carpal ligament and radial to the course of the median nerve. The motor branch to the thenar muscles can vary its anatomic pattern from the median nerve. Usually the motor branch comes off distal to the transverse carpal ligament, but occasionally it can branch proximal to it and pass below the ligament or over the ligament. Usually the motor branch comes off on the radial side of the median nerve, but rarely it branches on the ulnar side and passes superficial to the transverse carpal ligament. Appreciation of these anatomic variants by the surgeon is critical to ensure protection of the motor branch during surgical exposure. The distal branches of the median nerve supply sensation to the thumb, index, and long fingers and to the radial aspect of the ring finger.
Symptoms
Any condition that reduces space in the carpal tunnel can cause compression of the median nerve. Usually, compression is caused by flexor tenosynovitis. Although it has not been demonstrated that repetitive wrist motion can cause carpal tunnel syndrome, any activity that involves repetitive flexion or grasping can provoke symptoms, which include numbness or tingling in the median distribution and aching pain radiating to the forearm, elbow, or shoulder. Pain or paresthesia often awakens the patient at night. Symptoms can be triggered by position (wrist flexion) or repetitive grasping. Frequently, patients complain of clumsiness and loss of dexterity.
Clinical Evaluation.
The physical examination should include sensibility, motor, and provocative testing. Two-point discrimination is abnormal (>5 mm) in more advanced cases but can be normal in mild cases. Vibratory sensation may be a more sensitive test for detection of early carpal tunnel syndrome. Motor testing should include observing for thenar atrophy and testing abduction against resistance (abductor pollicis brevis). Provocative tests include those to elicit Phalen’s sign and Tinel’s sign.
Electromyography (EMG) can be used to confirm the diagnosis by demonstrating prolonged motor or sensory latency across the wrist. EMG testing is not necessary for patients who give a typical history and have appropriate physical findings. It is more useful for differentiating carpal tunnel syndrome from cervical radiculopathy.
Treatment
Conservative treatment consists of splinting, anti-inflammatory medication, and modification of activity. We use an off-the-shelf splint that maintains the wrist in a position of function in slight dorsiflexion. We recommend wearing the splint at night and as tolerated during the day. The splint may be removed as needed for essential activity. Local injection of a corticosteroid into the carpal tunnel may be effective. The appropriate technique of injection must be followed to avoid further injury to the nerve. Injection of corticosteroids is frequently transient in effect, and 60% to 90% of patients experience recurrent symptoms. Surgical treatment is indicated in patients who fail to respond appropriately to conservative treatment or when symptoms recur after an initial response.