In 1895, a Swiss surgeon, Fritz de Quervain, published 5 case reports of patients with tender thickened first dorsal compartments at the wrist. The condition subsequently has borne his name. De Quervain’s disease is an entrapment tendinitis of the tendons contained within the first dorsal compartment at the wrist, resulting in pain with thumb motion. It typically occurs in adults between 30 and 50 years old. Women are affected 10 times more frequently than men. The cause is almost always related to overuse, either in the home or at work, or is associated with rheumatoid arthritis. The presenting symptoms usually are pain and tenderness at the radial styloid. Sometimes a thickening of the fibrous sheath is palpable. Although Finkelstein’s test is probably the most pathognomonic objective sign, it is not diagnostic; the patient’s history and occupation, the roentgenograms, and other physical findings must also be considered. While trigger digit is the most common entrapment tendinitis in the hand and wrist, de Quervain tendinitis is the next most common, although it occurs approximately one twentieth as often as trigger digit.
Etiology
| The tendons of the abductor pollicis longus and extensor pollicis brevis are tightly secured against the radial styloid by the overlying extensor retinaculum. Any thickening of the tendons from acute or repetitive trauma restrains gliding of the tendons through the sheath. Efforts at thumb motion, especially when combined with radial or ulnar deviation of the wrist, cause pain and perpetuate the inflammation and swelling. |
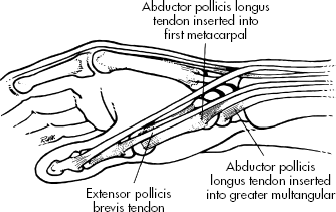 |
Signs and Symptoms
| Patients note pain with thumb and wrist motion and tender thickening at the radial styloid. Crepitation or actual triggering rarely is noted. Patients often are mothers of infants aged 6-12 months, and symptoms often are noted in both wrists. Repetitive lifting of the baby as it grows heavier is responsible for friction tendinitis. Day care workers, and others who repetitively lift infants, also are frequently affected. Those who have sustained a direct blow to the area of the first dorsal compartment also can develop de Quervain tendinitis. |
Examination
| The first dorsal compartment over the radial styloid is thickened and feels bone hard. This thickening usually distorts the sparsely padded skin in this area sufficiently to create a visible fusiform mass. The area is tender. The Finkelstein test (ie, flexion of the thumb across the palm and then ulnar deviation of the wrist; figure right) causes sharp pain at the first dorsal compartment (see figure). Tenderness is absent over the muscle bellies proximal to the first dorsal compartment. Tenderness and pain on axial loading are absent at the carpometacarpal (CMC) joint unless the patient has arthritis in that joint. | 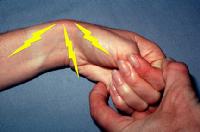 |
Treatment
Conservative treatment consists of rest in a splint, NSAIDs, and potentially the injection of a corticosteroid preparation. This is most successful within the first 6 weeks after onset. Harvey et al. reported 63 wrists initially treated with injections of steroids and local anesthetic into the tendon sheath. In 45 pain relief was complete (71.4%), and in 7 pain was relieved after a second injection. Only 11 (17.4%) required surgery. Christie in 1955, Lapidus in 1972, and Weiss et al. in 1994 reported similar experiences. When pain persists, surgery is the treatment of choice. Surgical treatment involves release of the first dorsal compartment on its dorsal side. Pitfalls of surgery include injury to the second branch of the radial nerve or failure to recognize and decompress the EPB lying in a separate compartment.
 |
|
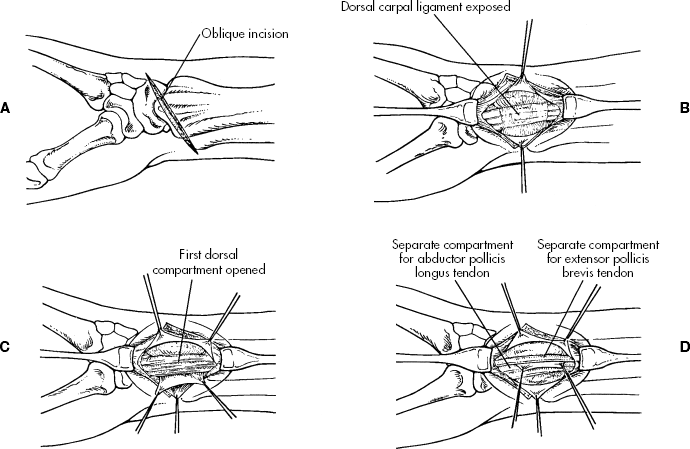
Figure: Surgical treatment of de Quervain disease. A, Skin incision. B, Dorsal carpal ligament has been exposed. C, First dorsal compartment has been opened on its ulnar side. D, Occasionally separate compartments are found for extensor pollicis brevis and abductor pollicis longus tendons.
|
It is important to note, when considering surgery, that anatomical variations are common in the first dorsal compartment. When the findings of anatomical dissections (Stein, Ramsey, and Key, Keon-Cohen, and Leão) are combined, 21% of patients displayed separate compartments. Reports of separate compartments found at surgery vary from 20% to 58%. More than half of patients may have “aberrant” or duplicated tendons, usually the abductor pollicis longus. These tendons sometimes insert more proximally and medially than usual, into the trapezium, the abductor pollicis brevis muscle, the opponens pollicis muscle, or the muscle fascia. The extensor pollicis brevis is considered a “late” tendon phylogenetically and is absent in about 5% of wrists. The presence of these variations and failure to deal with them at the time of surgery may account for any persistence of pain.

