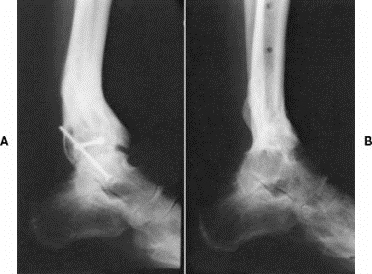
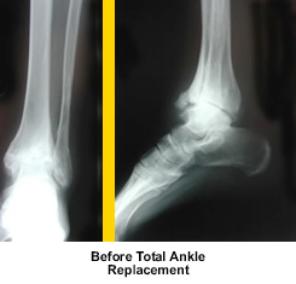
A) Post-traumatic arthritis B) Following tibiotalar arthrodesis (fusion)
Definition:
o Loss of tibiotalar joint space, destruction or degeneration of cartilage
Etiology of Arthritis:
o Posttraumatic
o Chronic degenerative, idiopathic (osteoarthritis)
o Inflammatory (rheumatoid)
o Septic (infection)
o Metabolic (gout)
Symptoms:
o Pain with weight-bearing
o Progressive and significant decrease in activity due to pain
Physical Exam:
o Decreased ankle dorsiflexion and plantarflexion (eversion and inversion are subtalar joint motions)
Radiographic findings:
o Joint space narrowing
o Subchondral sclerosis
o Osteophytes (spurs)
o Subchondral cysts
Surgical Treatment Options:
o Ankle Arthrodesis (fusion)
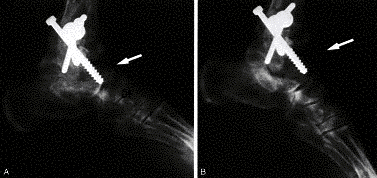
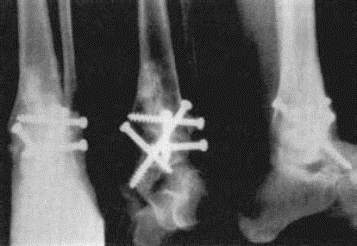
Post-op radiographs of ankle arthrodesis with distal fibula as biological plate
Motion following ankle (tibiotalar) fusion: Radiographs above demonstrate that dorsiflexion (DF) and plantarflexion (PF) motion in the subtalar and transverse tarsal joints is preserved and frequently increases to compensate for the lost tibiotalar motion
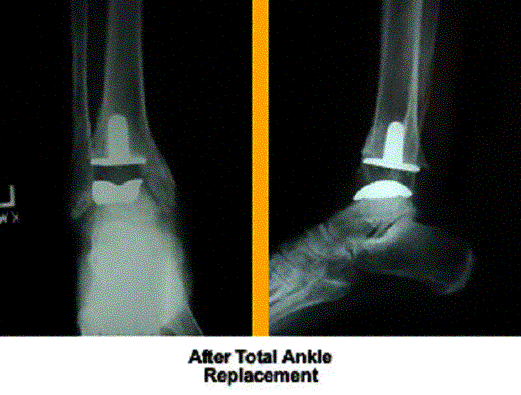
Ankle Arthroplasty (replacement)
Principles of arthrodesis:
Appose broad, cancellous, bony surfaces
Stabilize fusion with rigid fixation (eg screws)
Correct alignment of foot
Goals of arthrodesis:
Eliminate joint pain
Create stable, plantigrade foot
Ankle Arthroplasty:
Replaces ankle joint with metal prosthesis
Two main designs
Two-component fixed-bearing design
Three-component mobile-bearing design
Ankle arthroplasty not widely perfomed due to first generation failures in the 1970’s
Ankle soft tissues are thin, easily compromised by previous trauma, surgery, disease, or steroid use
Delayed wound healing in up to 40% of patients
Deep infection rates between 3-5%
New generation prostheses claim improved implant survival
Not yet FDA approved