dry, scaly, swollen, clumsy limb that the patient dissociates from the rest of the body because of the loss of sensory feedback
Pathophysiology
Breakdown of the skin
Stems from diminished sensation from neuropathic disease
Trauma from unappreciated local stress on feet
Autonomic neuropathy dries and cracks skin, exposing to infection
Autonomic neuropathy impedes normal reactive hyperemia
Motor neuropathy affects intrinsic muscles leading to deformities and bony prominences which predispose to ulceration
Exacerbated by diabetic co-morbid conditions:
Peripheral atherosclerosis impedes oxygen delivery to distal tissue
Compromised microvasculature diminish likelihood of wound helaing
Nephropathy leading to peripheral edema, stasis
Text Box: Wagner Classification of diabetic foot ulcers:
o Grade 0—skin intact but bony deformities produce a “foot at risk”
o Grade 1—localized, superficial ulcer
o Grade 2—deep ulcer to tendon, bone, ligament, or joint
o Grade 3—deep abscess, osteomyelitis
o Grade 4 – gangrene of forefoot
o Grade 5 – gangrene of entire foot
Retinopathy causing inability to see and care for feet
Physical Exam:
Inspection of skin, hair growth, perfusion, pulses, color
Bony prominences
Metatarsal heads
Dorsum of proximal interphalangeal joints
Medial arch in Charcot foot (see below)
Neurologic exam
Light touch, Pin-prick, Vibration, Proprioception
Vascular exam:
Palpation of pulses
Determination of Ischemic Index
Brachial artery blood pressure ¸ dorsalis pedis and posterior tibial arteries blood pressure
Normal = 1, Index >0.45 – 90% of ulcers will heal
Limitation of Ischemic Index is inability to determine pressure calcified and sclerotic lower extremity vessels
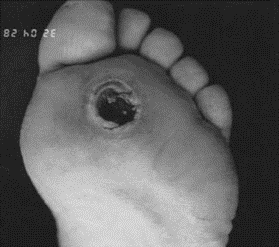
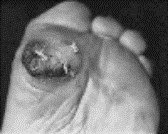
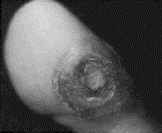
Grade 3 Ulcer, exposed metatarsal head, presumed osteomyelitis
Early neuropathic arthropathy with dislocation of first and second metatarsocuneiform articulations, but without significant bony
Treatment of diabetic ulcers:
A multidisciplinary team approach to treatment is crucial, involving a dietician, endocrinologist, infectious disease specialist, vascular surgeon, orthopaedic surgeon, diabetic nursing specialist, orthotist, prosthetist, and podiatrist
Dependent on determining if the ulcer is:
primarily neurotrophic or ischemic
localized or heralds a deep abscess
osteomyelitis or pyarthrosis is absent or present
Neuropathic Arthropathy – Charcot Foot
Etiology:
** Diabetes
Also – Hansen Disease, Neurosyphiis, Paraplegia, Alcoholism, Syringolmelia, Myelodysplasia
Hypothesized Pathophysiology:
1. Loss of autonomic control of vasculature
Increased blood flow 5 times normal
Results in osteopenia
2. Combined with somatic sensory loss of pain and proprioception
3. Minor injury (often unnoticed) with resulting localized warmth and swelling out of proportion to injury
4. Eventual bony dissolution and loss of structural integrity, collapse deformity
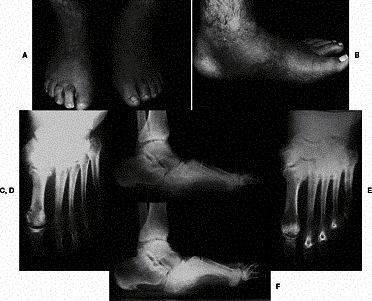
A & B, Acute inflammatory stage: swelling and loss of arch, warm, dry, and nontender and had midfoot crepitance. C, dissolution of bone at Lisfranc articulation. D profound collapse deformity. E and F, 3 years later.
Treatment:
Inflammatory stage:
Characterized by acute, warm, swollen foot
Immobilization is key
Non-weightbearing cast until all signs of inflammation resolve
(Often inflammatory stage progresses to collapse deformity prior to presentation)
Early deformity:
Subluxation of tarsometatarsal joint without significant soft-tissue or bony destruction
Closed, percutaneous pinning or open reduction internal fixation (vs arthrodesis) followed by cast immobilization and non-weightbearing
Late deformity:
Padding of bony prominences, custom orthothotics,