Overview
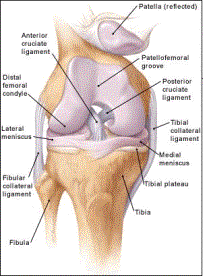
The anterior cruciate ligament is a very common injury with an estimated 100,000 new ACL injuries reported each year in the United States. It is a very common sports related injury in both men and women athletes. However, ACL injuries are 2-8 times more common in female athletes than in men competing in the same sports. The increased risk in female athletes is felt to be multifactorial with both intrinsic (anatomic differences, increased joint laxity/flexibility, hormonal influences) and extrinsic (muscle strength, neuromuscular control, knee stiffness, landing characteristics, posture control) causes.
The femoral attachment of the ACL is at the posterior inner surface of the lateral femoral condyle. The fibers of the ACL fan out as they insert onto the tibia. The ACL inserts onto the tibia just lateral to the medial intercondylar tubercle.
The ACL is the primary ligament responsible for limiting anterior tibial translation. Ligament cutting studies have shown that the ACL contributes to 80-85% of total resistance to anterior translation. These studies have also shown that there is more translation of the knee at 30º than at 90º of knee flexion after sectioning of the ACL. The ACL has also been shown to be a secondary stabilizer of tibial rotation and varus/valgus stability.
The classic “terrible triad” of the knee was originally described as in injury to the ACL, medial collateral ligament, and the medial meniscus. More recent literature has shown that the lateral meniscus, not the medial meniscus, is more likely to be injured in the acute ACL tear. Medial meniscal tears are more common in the chronic ACL injury.
History
The classic history of an isolated ACL tear is described in a patient that injures his/her knee with a non-contact sudden stopping, cutting or jumping mechanism. Historically, if a patient describes a “pop” at time of injury and has a notable hemarthrosis, there is a 70% likelihood that the patient sustained an ACL injury. ACL injuries can also occur with contact injuries. Contact injuries more often result in multi-ligamentous injuries.
Patients with chronic ACL injuries will often present to clinic with recurrent episodes of instability. They will often remember their initial injury. Patients with clinically significant chronic ACL injuries will complain of their knee giving way and swelling with certain activities.
Physical Exam
It is important to complete a full physical exam of the knee. There is often other pathology associated with ACL injuries including meniscal tears (60%), osteochondral fractures (10-20%), and other ligament injuries of the knee (20%).
Lachmans test of the knee
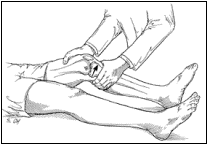
The most common provocative maneuvers used for assessing the ACL are the Lachman, anterior drawer, and pivot shift tests. With all three testing maneuvers, it is extremely important to compare the injured knee to the contralateral side. The Lachman test is considered the most reliable test for assessing an ACL injury. The Lachman is performed by flexing the knee to 30º and the tibia is translated forward while the thigh is stabilized. A positive Lachmans test will demonstrate increased anterior tibial translation and will lack a firm endpoint. The anterior drawer test is performed in a similar fashion as the Lachmans except testing is done at 90º instead of 30º. The pivot shift test is performed by first placing the knee in full extension. An ACL deficient knee will be subluxated in full extension. The tibia is then externally rotated and a slight valgus load is applied to the knee as it is brought into a flexed position. A positive pivot shift will result when the anteriorly subluxated tibia reduces posteriorly as the knee is brought into a flexed position.
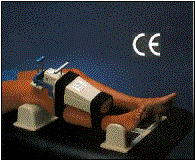
ACL laxity can also be tested with the use of a knee arthrometer. It is particularly useful in patients that are difficult to examine secondary to pain or guarding. The arthrometer can measure anterior translation of the tibia. If the arthrometer measures greater than 10mm of maximum translation or shows more than 3mm greater translation compared to the contralateral knee, than a diagnosis of an ACL rupture is highly suspect.
Knee Arthrometer: KT 1000
Imaging
Plain radiographs should be obtained in all patients with a suspected ACL injury. One finding on the AP radiograph that is important in the work up of an ACL injury is the Segond fracture. This is an avulsion fracture of the lateral capsule off the lateral tibial plateau. This is pathognomonic for an ACL injury. However, more commonly the radiographs will appear normal but it is extremely important to rule out other possible bony injuries.
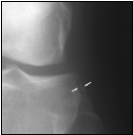
Segond Fracture
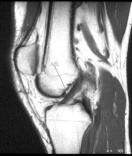
MRI: Intact ACL
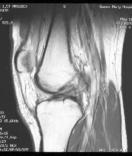
MRI: ACL tear
It is not necessary to obtain an MRI for the workup of an ACL injury although the study may be helpful in identifying other potential injuries. In addition to identifying ACL tear, other common findings include bone bruises in the lateral femur and tibia and meniscal injuries. For most isolated ACL injuries, an MRI does not change the diagnosis or treatment plan. An MRI may be more helpful in multiligamentous injuries.
Treatment
The treatment plan after an ACL injury should consider the age, activity level, and activity type of the patient. Younger active individuals tend to do poorly with non-operative treatment. Younger patients tend to have more recurrent episodes of instability and over time can significantly damage the knee leading to early degenerative arthritis. Patients that wish to continue participating in cutting sports (football, soccer) also tend to do poorly without operative management. It is generally recommended that young, active patients undergo ACL reconstruction.
Non-operative management is a viable option in the treatment of the ACL deficient knee. Non-operative treatment consists of physical therapy and a knee strengthening program, activity modification, and protective bracing. Non-operative management tends to be more successful in the older population.
Schematic ACL reconstruction