Anatomy
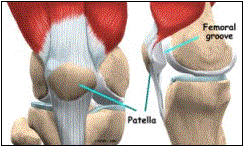
The patella is a sesmoid bone located within the quadriceps tendon. The patella articulates directly with the distal femur forming the patellofemoral articulation. It increases the mechanical advantage of the quadriceps by increasing the functional lever arm. The patella is kept centered within the femoral trochlear groove by many soft tissue stabilizers including the quadriceps tendon, patellar tendon, lateral retinaculum, and the medial patellofemoral ligament. The most important medial stabilizer of the patella is the medial patellofemoral joint. It provides approximately 50% of the lateral restraining force.
Etiology
Patellar dislocations may occur with a direct trauma to the knee or an indirect twisting of the knee. The patella tends to displace laterally with dislocation events. The typical age for patellar dislocations is between 15-20 years of age and is more common in females.
There are numerous risk factors for patellar dislocations. These include a shallow patellofemoral groove, patella alta, an increased Q-angle, ligamentous laxity, genu valgum, rotational malalignment of the lower extremities, and muscle imbalance.
History/Physical Exam
After an acute patellar dislocation, the patella will often reduce spontaneously. Occasionally, the patella will not reduce by itself and acute management is necessary. Patients will complain of a giving way of the knee at time of injury.
On physical exam after acute dislocation, there is usually an effusion. Flexion will be limited secondary to pain. Patients will have tenderness along the medial aspect of the patella and will be apprehensive when attempting to translate the patella laterally (patellar apprehension sign). It is important to do a thorough exam of the lower extremities to assess for other injuries.
With chronic patellar dislocations, patients will report multiple events of subluxation or dislocation. On exam, the overall alignment, patellar mobility, patellar tracking, and apprehension are just a few physical findings that should be assessed.
Imaging
Merchant view: patellar dislocation

MRI: acute tear of the medial patellofemoral ligament
The radiographic evaluation begins with an anteroposterior, lateral and Merchant view of the involved knee. The Merchant view provides an axial image of the patellofemoral joint. The radiographs are often normal but occasionally osteochondral fractures may be seen on the medial patellar facet or the lateral femoral condyle. Lateral subluxation of the patella may also be seen secondary to the disrupted medial restraints.
An MRI may be obtained to further assess the knee. The MRI can help identify osteochondral injuries and the site of rupture of the medial patellofemoral ligament as well as other concomitant injuries.
Treatment
If the patella remains dislocated after injury, the patella should be reduced immediately. More commonly the patella will spontaneously reduce. Once reduced, the knee should be treated in an extension immobilizer to allow healing of the torn medial structures. Rehabilitation should concentrate on medial quadriceps strengthening and stretching of the lateral structures. First time dislocators have a 20-44% chance of redislocating with non-operative treatment. Some have recommended acute repair of the medial patellofemoral ligament although this is controversial.
Despite non-operative measures, some patients continue to have recurrent episodes of instability and persistent anterior knee pain. Surgical options are numerous and include proximal realignment, distal realignment and medial patellofemoral ligament reconstruction. Proximal realignment procedures involve a quadricepsplasty and are designed to alter the pull of the quadriceps muscle to a more medially directed force. Distal realignment procedures require a tibial tubercle osteotomy and displacement of the tubercle to a more medial position. The medial patellofemoral ligament reconstruction uses a soft tissue graft to re-create the medial patellofemoral ligament and restore the primary restraint to lateral translation.

