Overview
The shoulder is the most mobile joint in the body. The glenohumeral joint is rather shallow and only 25-30% of the humeral articular surface comes into contact with the glenoid at one time. The shoulder relies on static and dynamic soft tissue constraints for stability. Due to the increased mobility of the glenohumeral joint and lack of bony constraints, the shoulder is quite susceptible to dislocation.
Anterior Dislocations
AP shoulder: anterior dislocation
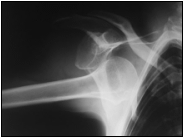
Anterior dislocation of the shoulder is the most common type of shoulder instability. Anterior dislocations occur following a load to the shoulder in an abducted, externally rotated position.
Patients will present with pain of the shoulder and guarded motion. On presentation, the arm is typically held in abduction and internal rotation. It is important to obtain a thorough neurovascular exam, particularly of the axillary nerve. Prior to reduction maneuvers, radiographs of the shoulder should be obtained to assess for associated fractures and the direction of the dislocation. There are numerous methods described for relocation of the shoulder.
Initial treatment of the first time dislocator should be non-operative management with initial reduction and immobilization followed by progressive range of motion and a strengthening program. Reasons for acute surgical management include irreducible reductions and large glenoid rim fractures displaced >5mm or greater than 25% of the articular surface.
Anterior shoulder dislocations have associated injuries. In the younger population, anterior dislocations are most commonly associated with a Bankart lesion (avulsion of the inferior glenohumeral ligaments, the labrum and the capsular attachment with or without an avulsion of the glenoid rim). Older patients that sustain an anterior shoulder dislocation tend to have associated rotator cuff tears.
Apprehension Test
The prognosis of recurrent shoulder dislocations is dependant on patient age and activity level. The younger, more active patients are more likely to redislocate. Studies have reported recurrence rates of 70-95% in patients under 20 years old. Patients over the age of 40 rarely have recurrent dislocations.
Recurrent dislocators should be treated with surgical management if rehabilitation and activity modification is not successful. Patients will provide a history of recurrent subluxation or dislocation events or report a feeling of a dead arm and looseness of the shoulder. Clinical findings in these patients include a positive “apprehension sign”. The patient is noted to be apprehensive when placed in an abducted externally rotated position. A repair of the Bankart lesion may be done either with open or arthroscopic techniques. Both techniques address repair of the anteroinferior capsulolabral complex.
Posterior Dislocations
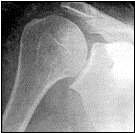
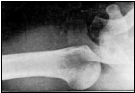
AP & axillary lateral shoulder: posterior dislocation
Posterior dislocations are rare and account for approximately 2% of all shoulder dislocations. Mechanisms for posterior dislocations include a posteriorly directed force on a forward flexed arm, seizures and electrocution injuries. During seizures and electrocution injuries, the internal rotators of the shoulder forcefully contract and overpower the weaker external rotators and direct the shoulder posteriorly. Posterior shoulder dislocations are a commonly missed injury. Patients present with an adducted internally rotated arm. On an anteroposterior radiograph, the proximal humerus is often located directly posterior of the glenoid and may appear “located”. It is essential to obtain an axillary lateral view to assess a dislocation. Initial treatment includes reduction and immobilization.
Recurrent posterior dislocators often report difficulty using their arm in a forward flexed, internally rotated position. The patient will complain of pain or apprehension if placed in this position with the shoulder loaded in a posterior direction. Shoulder radiographs should be reviewed for bony injuries including reverse Bony Bankart lesions (posterior glenoid avulsions), lesser tuberosity fractures, and reverse Hill-Sachs lesions (compression fracture of the anteromedial humeral head). Surgical treatment of recurrent posterior dislocations may be addressed arthroscopically or with open techniques of the posterior capsulolabral complex. There are numerous open techniques described for treatment of the chronic unreduced posterior dislocations.
Multidirectional Instability
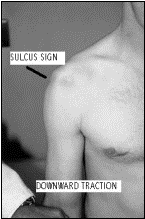
Multidirectional instability refers to shoulder ligamentous laxity with instability in multiple directions. These patients tend to have bilateral shoulder laxity. At risk populations include gymnasts, swimmers, overhead athletes and those with collagen disorders. Physical findings include increased translation of the shoulder in the anteroposterior plane and a positive sulcus sign.
Rehabilitation with a shoulder strengthening program is the primary mode of treatment. In general, MDI is not well suited for operative management. If non-operative treatment fails, then an inferior capsular plication may be performed to tighten the capsule laxity. Operative results of MDI tend to be inferior to the success rates of unidirectional instability procedures.

