The giant cell tumor (GCT) is a mostly benign lesion that is classically known for the presence of numerous giant cells. However, giant cells are also frequently encountered in other tumors that include anuerysmal bone cyst, solitary bone cyst, chondroblastoma, osteoblastoma/osteoid osteoma, and hemorrhagic osteosarcoma. Giant cells are also frequently noted in chronic exposure to foreign bodies and certain infections (TB & coccidiomycosis). The further confuse the matter; there also exist two benign variants in the hand. These include Giant Cell Tumor of Tendon Sheath and Giant Cell Reparative Granuloma. Finally, the Brown Tumor of hyperparathyroidism is considered to be a GCT variant. In this section, we will focus on the classic giant cell tumor only.
GCT predominates in the 3rd decade and has a female predilection. Most tumors are found about the knee (50%) but are also commonly found in the distal radius and sacrum. Symptoms are usually mild or absent until levels of cortical destruction produce a pathologic fracture. The GCT is capable of producing a knee effusion in the absence of trauma; which can often be the only presenting sign. GCT is known as a benign tumor with rare malignant characteristics. One percent are known to metastasize to the lungs and carry a grim prognosis and 6% will recur following resection.
Radiographically, GCT is markedly lytic and is one of the few tumors known to involve the epiphyseal regions of long bones (Figure #20,21). The metaphysis can also be involved and the tumor will grow towards the joint until it contacts the articular cartilage. GCTs are not known to penetrate articular cartilage. Pulmonary staging is imperative and includes chest CT before any further work-up is complete.
The risk of malignant transformation in these tumors is low (<5%) unless XRT has been undertaken. Doses of >3000 cGy have been associated with rates of 15-20% malignant transformation. For this reason, current therapies involve aggressive curettage, phenol adjuvant, and cement placement for structural support. With this modality a recurrence rate of 10-25% should be expected, making frequent follow-up a must. In addition, Chest X-rays should be followed every 6-12 months for 3 years. Lesions that involve the proximal fibula can be resected completely with relative impunity.
Figure # 20
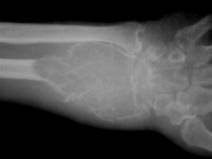
Giant Cell Tumor of the distal radius
www.thachers.org
Figure # 21
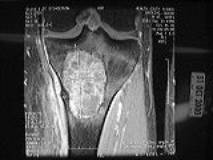
MRI of the proximal tibia showing a Giant Cell Tumor
www.sarcoma.org

