Clavicle Injuries
The Clavicle is the first bone to ossify (between the fifth and sixth weeks of fetal life), and the last bone in which physeal closure is observed (approximately 25 years of age). Fractures of the clavicle can occur in any age group, from neonate to adult, and can involve any portion of the clavicle from sternum to acromion.
Fractures of the clavicle at the time of birth are the most common fracture in newborns. Generally, the diagnosis is made by the pediatrician when observing an asymmetric Moro reflex, and/or the child’s unwillingness to move the affected upper extremity, termed pseudoparalysis. Great care must be taken to rule out coincident brachial plexus injury. Treatment is typically non-operative with immobilization of the affected limb to the chest wall, and long-term sequelae are extremely rare.
In the growing child, clavicular shaft fractures are one of the more commonly observed skeletal injuries. History usually includes a fall on the point of the shoulder, and the presence of tenderness and swelling around the mid-clavicle will generally allow for prompt diagnosis. Most of these fractures will be of the greenstick variety. Immobilization with a sling and swathe or figure of eight brace will usually suffice for treatment. Callus healing will often lead to a visible and palpable bump in the region of healing, and can cause alarm in caregivers that have not been properly forewarned.
Fractures of either the medial or distal ends of the clavicle often include some degree of physeal involvement, and should be carefully evaluated. Again, sling and swathe immobilization will adequately protect against re-injury, and will allow satisfactory healing. On very rare occasion, posterior displacement of medial physeal injury is observed, and sometimes requires open reduction and fixation to prevent risk to the contents of the thoracic cavity.
Proximal Humerus Injuries
Proximal humerus fractures represent less than 5% of children’s fractures. These can be physeal injuries. It is important to understand the normal radiographic anatomy of the proximal humeral physis, so that the diagnosis can be made accurately, and the degree of physeal involvement can be assessed. This physis is not planar, but rather is tent-shaped, with the apex posteromedially. Under age 5, these injuries are typically Salter-Harris type I, whereas after age 11, they are typically SH type II.
In the newborn sub-population, proximal humeral injuries can be challenging to diagnose, given the preponderance of cartilage in this region, and the resultant radiolucency. This injury is common in the newborn nursery as a result of birth trauma, and can manifest itself as pseudoparalysis. Fortunately, nonoperative treatment is usually adequate. This is due, in part, to the fact that 80% of humeral growth occurs proximally, allowing tremendous remodeling potential. In fact angulation of up to 45° will have disappeared by 6 months of age.
Goals of reduction include angulation less than 45° and displacement of less than 70%. If adequate reduction is possible, non-operative treatment will yield acceptable results. In very rare cases, where reduction cannot be maintained, percutaneous pinning may be required, though usually only in children over age 12.
Spiral fractures of the humeral shaft are an entity worth mentioning. Particularly in the child under three years old, the torsional mechanism required to create this mode of failure, is often telling of child abuse. In fact, about 80-90% of shaft fractures in children under 3 are thought to be due to abuse.
Fractures About the Elbow
Radiographs
The standard radiographs of the elbow include an anteroposterior view with the elbow extended and a lateral view with the elbow flexed to 90° and the forearm neutral. If a line is drawn along the anterior border of the distal humeral shaft, it should pass through the middle third of the ossification center of the capitellum. This is referred to as the anterior humeral line. A line directed proximally along the anterior border of the coronoid process should barely touch the anterior portion of the lateral humeral condyle. This is called the coronoid line. A line drawn down the shaft of the radius should pass through the capitellum. This is called the radiocapitellar line. Because of the ever-changing ossification pattern, identification and delineation of fractures about the elbow in the immature skeleton may be subject to misinterpretation. Some vagaries of the ossification process about the elbow may be interpreted as a fracture. It is therefore imperative to understand the relative time interval of formation of each of the six ossification centers around the elbow. The ossification center of the capitellum appears first at about 6 months. At intervals of roughly 2 years the remaining ossification centers form in the following order; radial head, medial epicondyle, trochlea, olecranon, lateral epicondyle
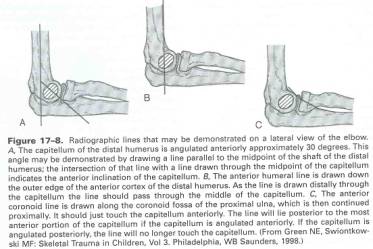
Other important radiographic findings to be familiar with include the fat pad sign. There are fat pads that overlie the capsule in the coronoid fossa anteriorly and the olecranon fossa posteriorly. Because of their location deep within these fossae, they are generally not visible radiographically. in the presence of a joint effusion, however, displacement of either or both of these fat pads may become apparent. Presence of a posterior fat pad sign is the most telling, and should be considered a fracture until proven otherwise.
Supracondylar Humerus Fractures
Children often extend their elbows to break the force of a fall. Because of ligamentous laxity, the elbow hyperextends, allowing the linear force applied along the extended elbow to be converted to a bending force. This bending force is then concentrated by the olecranon into the anatomically weak supracondylar area producing a supracondylar fracture. As extension type (98%) supracondylar humerus fractures are far more common than flexion type (2%), we will focus on them here.
Age is the key factor in the incidence of supracondylar fractures. This fracture, without intra-articular extension, is almost exclusively a phenomenon of the immature skeleton. Incidence increases during the first 5 years and peaks at 5 to 8 years of age. After this, there is a decrease in incidence until age 15, after which it is rare. This decrease in the incidence of supracondylar fractures is replaced by a rising incidence of elbow dislocations. Males sustain almost twice as many supracondylar fractures as females
.
Nerve injuries occur in about 8% of these extension-type injuries. The most commonly injured is the anterior interosseous, followed by the radial and ulnar in descending order. The ulnar is the most common injured nerve in flexion-type supracondylar fractures.
Vascular injury is another significant concern in treating these fractures. The brachial artery is particularly susceptible to injury in hyperextension type injuries, and can lead to a compartment syndrome. Undiagnosed and prolonged compartment syndromes of the forearm can cause a specific clinical entity known as Volkmann’s ischemic contracture, though this has been described as occurring in only 0.5% of cases (and even far fewer in a recent conference poll of many of our pediatric staff). Historically, these injuries were treated with casting in hyperflexion, which led to a high rate of Volkmann’s contracture, but with the advent of percutaneous pinning techniques (see below), the arm could now be immobilized at 70-80 degrees of flexion yielding markedly decreased rates of this complication.
Gartland’s classification is a simple system that is widely accepted. In type I injuries the fracture is non-displaced or minimally displaced such that the anterior humeral line still passes through the ossification center of the capitellum on the lateral radiograph. In type II injuries there is an obvious fracture line with displacement of the distal fragment, but there is still an intact cortex posteriorly. In type III injuries the fragments are completely displaced.
Non-displaced, or type I, supracondylar fractures usually require no more than simple immobilization for comfort and further protection. Once the neurovascular assessment is made, placing the extremity in either a posterior splint or circular cast is all that is necessary. The decision of whether to hospitalize the child for a brief period of observation usually depends on the degree of soft-tissue swelling and discomfort and the reliability of the parents. By 3 weeks after injury, the pain and swelling usually have significantly subsided to allow a protected active range of motion. X-ray evaluation at this time usually reveals periosteal new bone formation in the supracondylar area of the humerus.
Treatment of type II fractures involves relaxation of the patient, manipulation and casting or splinting. Sometimes percutaneous fixation is necessary to prevent the deformity from recurring or to avoid the need for immobilization in more than 70 or 80° of flexion. Adequate relaxation often requires a general anesthetic, so as to allow the surgeon to better manipulate the fracture fragments. Manipulation is carried out with the goal of approximating the carrying angle of the uninjured side. Hyperflexion with the arm in a fully pronated position will generally reduce these fractures. Maintaining this reduction, can be challenging as the arm should remain in a position of 125-135 degrees of flexion. if there is any concern regarding the degree of swelling, and the added vascular compromise that this may impose, one should not hesitate to consider percutaneous pin placement for added stability, allowing the arm to be held in 90 degrees or less of flexion.
Treatment of type III injuries must follow the following three steps. First, there must be some type of manipulation to obtain a reduction of the fracture. Second, once the fracture is reduced, the quality of the reduction must be assessed. And third, the reduction must be maintained until the fracture is healed enough to be intrinsically stable. Historically, there are many different approaches to treatment of these injuries, but for the sake of simplicity, we will herein discuss only the gold standard, percutaneous pin fixation with splinting or casting.
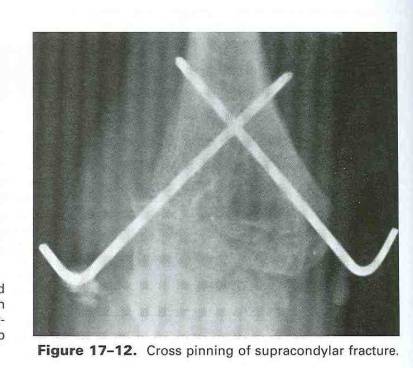
Stabilization of reduced type III fractures with pins placed percutaneously has become the universally accepted method of treatment. Pins may be placed from medial to lateral, lateral to medial, or both. Most surgeons will elect to place either 1) crossing k-wires, one from each side or 2) parallel pins placed lateral to medial (which helps avoid injury to the ulnar nerve, but compromises some amount of stability). In particularly unstable fracture patterns, many will elect to place two parallel lateral to medial pins, and a third medial to lateral that crosses these first two.
Incidence of injury to the ulnar nerve is estimated to be 2% to 3%. In the reports of ulnar nerve injury occurring after pin fixation, most cases will clear spontaneously after removal of the offending pin.
Further management generally consists of three or four weeks of immobilization, followed by removal of pins in the office, and active range of motion started at the child’s own pace. Strategies for prevention of reinjury include continued splinting during play, or simple sling use for an additional 3-4 weeks time, or until tenderness resolves and the child has begun to use the arm freely without difficulty.
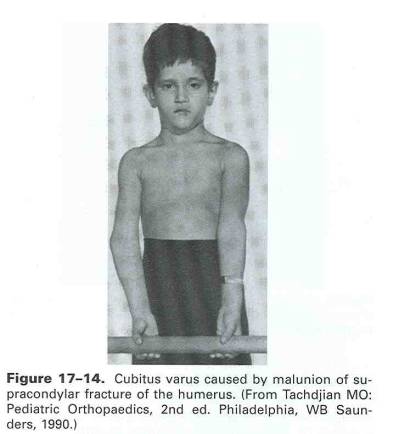
Cubitus varus (figure 17-14), or varus angulation through the region of the elbow, is the most common late deformity associated with a supracondylar humerus fracture. Typically it is caused by malreduction or failure to maintain an adequate reduction, but can also occur due to osteonecrosis of the trochlea. If the deformity is excessive, and is cosmetically objectionable to the patient and family, a corrective supracondylar osteotomy can be performed.
Condylar Fractures
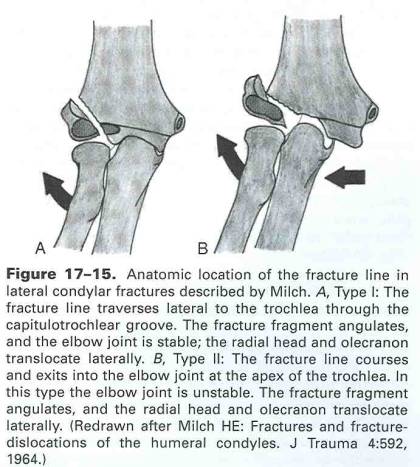
Fractures of the lateral condylar physis constitute about 17% of fractures of the distal humerus. Fractures involving the lateral condylar region in the immature skeleton either cross the physis (Milch type I) or follow it for a short distance into the trochlea (Milch type II). The diagnosis of these injuries may be less obvious both clinically and radiographically than that of supracondylar fractures, especially if the fracture is minimally displaced. These injuries are a challenge to treat, and typically have worse outcomes than suprcondylar injuries due to the poor blood supply of the fracture fragment, and because they are intra-articular and transphyseal.
Fractures of the lateral condylar physis are only occasionally associated with injuries outside the elbow region. Within the elbow region, the associated injuries that can occur with this fracture include dislocation of the elbow (which may be a result of the injury to the lateral condylar physis rather than a separate injury), fractures of the radial head, and fractures of the olecranon, which are often greenstick in nature.
The incidence of a functional loss of range of motion in the elbow is considerable with fractures of the lateral condylar physis because the fracture line often extends into the articular surface. A difficult supracondylar fracture with cubitus varus, barring the immediate neurovascular complications, is likely to result in a surgically correctible cosmetic deformity with an essentially normal range of motion in the elbow. A poorly treated lateral condylar physeal injury, however, is likely to result in a significant loss of range of motion that is not as responsive to surgical correction.
A Milch Type I lateral condylar injury is a true Salter-Harris type IV injury through the ossific nucleus of the lateral condyle. In this type, the fracture line originates in the metaphysis, crosses the physis more or less obliquely, and finally traverses the ossification center of the lateral condylar epiphysis to exit in the area of the capitulotrochlear groove. A Milch Type II injury is more common, and shares characteristics of both Salter-Harris II and III type physeal injuries. The most common fracture line originates in the posterolateral metaphysis, where there is a fragment of variable size. The fracture then usually courses within the physis down to the depths of the trochlea. In this most common type, the fracture line does not traverse the lateral condylar epiphysis or ossification center. The ossification center of the lateral condyle extends to the lateral crista of the trochlea. Thus, the terminal portion of the fracture line courses through the physeal cartilage that lies between the ossification centers of the lateral condyle and the medial condyle. Treatment guidelines follow those of a type IV injury: open reduction and internal fixation of displaced intra-articular fractures, with the potential for mild growth disturbance of the distal humeral physis.
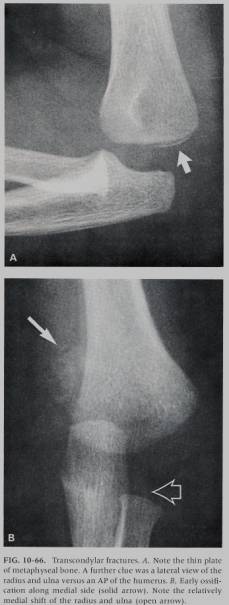
Notice in figure 10-66 how such a small sliver of bone can actually represent a larger fracture when considering the non-ossified portions of the distal humerus.
There are three alternatives for managing fractures involving the lateral condylar physis: simple immobilization alone, reduction by closed methods, or open surgical reduction.
Minimally displaced fractures are stable and have considerable intrinsic soft-tissue attachments that prevent displacement of the distal fragment. About 20% of lateral condylar physeal fractures are sufficiently nondisplaced that they can be treated by simple immobilization without surgical intervention
Because of the high incidence of poor functional and cosmetic results with closed reduction methods, open reduction has become the most widely advocated method for unstable fractures with appreciable displacement. Smooth pins are the most popular method of fixation.
Fractures of the medial humeral condyle occur with about half the frequency of lateral condyle injuries. This is generally an avulsion type injury, and can often be associated with elbow dislocation. As such is the case, after reduction of an elbow dislocation, it is very important to check post-reduction films to be sure that there are no bony fragments of a medial condyle fracture that have become entrapped in the joint.
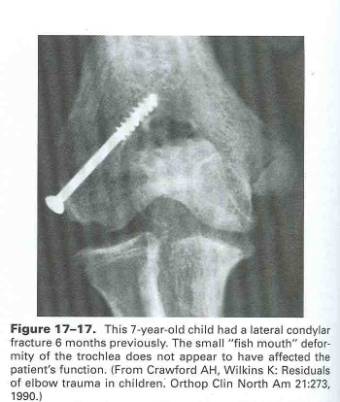
These injuries were also classified by Milch, and are divided into three types. Type I fractures begin in the metaphysis and traverse the apex of the trochlea. Type II injuries start in a similar manner and exit the groove between the capitellum and trochlea. Type III injuries can be either of these types with significant displacement or rotational mal-alignment. Displacement over 5mm is usually an indication for operative management, and generally smooth pin placement is the procedure of choice, though screw fixation is preferred by some (see figure 17-17)
Proximal Radius Injuries
Injuries to the proximal radius make up about 10% of fractures about the elbow. Usually, the insult is to either the radial neck or the proximal radial physis. These injuries are graded based on the degree of angulation, though it is most important to remember simply that somewhere between 15 and 30 degrees of angulation is the upper limit of acceptability for most authors. Closed reduction should be attempted first, but failing that, consideration can be given to percutaneous pinning. With any proximal radial injury, the ulna should be very closely evaluated to rule out plastic deformation suggestive of a Monteggia type injury (see below). As a rule, the posterior border of the ulna should be completely straight. Any deviation from this should be considered bony injury.
Forearm Injuries
Forearm fractures account for about 45% of fractures in children. Approximately 75% occur in the distal third, 20% in the middle third and 5% in the proximal third. Most forearm fractures in children are the result of a fall on the outstretched hand. Often the abbreviation FOOSH will be used in medical documentation to indicate this mechanism of injury. Generally the arm is in a position of relative pronation, and the fall creates a supination force, resulting in the commonly found apex anterior supinated deformity.
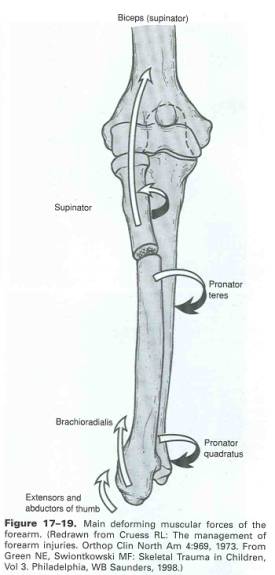
In evaluating forearm fractures, the deforming muscular forces should be kept in mind to help understand the reasons for the presenting radiographic and clinical appearance, and treatment rationale (figure 17-19). Distal fractures are often deformed by the brachioradialis, while middle third fractures are more involved. The supinator and biceps tend to flex and supinate a proximal radius fragment, while the pronator teres can serve to pronate a distal radius fragment. Knowing these muscular insertions, can aid in reduction maneuvers, and can help in the planning of immobilization.
As with all orthopedic injuries, forearm injuries should be evaluated with radiographs of the joint above and the joint below the injury to be certain that elbow and wrist involvement are not missed.
In general, forearm fractures can be treated non-operatively in a long arm cast with satisfactory results reported in about 85% of cases. Reports of loss of pronation and supination have however turned the tide of management options somewhat, and have led to increasing enthusiasm for operative management.
Some specific forearm injuries that warrant further attention include distal radial physeal injuries, Monteggia fracture dislocations and Galeazzi fracture dislocations.
Distal radial physeal injuries are the most common physeal injuries incurred by juvenile long bones. 75% occur around the onset of puberty. Most of these are Salter-Harris II type injuries, though in younger children, they tend to be of the Salter-Harris I type. Frequently, they can be treated non-operatively with closed reduction and casting. Most authors will start with long-arm casting and progress to short arm casting once callus formation is visible radiographically. Partial or complete growth arrest is observed in 5-10% of cases.
Monteggia Fractures
First described by Giovanni Battista Monteggia in 1814, fracture dislocations involving dislocation of the redial head accompanied by a proximal ulna fracture, are termed Monteggia fractures. The ulnar fracture can be complete, incomplete or just plastically deformed. Jose Luis Bado worked extensively in further characterizing these injuries, and gave us a simplified classification system based on the mechanism of injury.
A Bado type I injury involves an anterior dislocation of the radial head with a fracture of the ulnar diaphysis. This represents about 70% of all Monteggia lesions in pediatric populations. The type II lesion is a posterior dislocation of the radial head associated with an ulnar diaphyseal or metaphyseal fracture with posterior angulation. It is uncommon in children, with most of the early series categorizing this as a fracture of adults only. The type III lesion consists of a lateral or anterolateral dislocation of the radial head associated with a fracture of the ulnar metaphysis. In children, the metaphyseal fracture is generally of the greenstick variety. This pattern represents about 23% of the lesions in children and is, therefore, the second most common type of Monteggia fracture in children. It is often associated with radial nerve injuries. The type IV Monteggia lesion, also rare in children, is the association of anterior dislocation of the radial head, fracture of the middle third of the radius, and fracture of the ulna at the same level as, or more proximal to, the radius fracture.
Associated Nerve Injuries
There is a close relation between the posterior interosseous nerve and the proximal radius, as the nerve comes anterior and anterolateral to the radial head and neck on its path through the supinator muscle. With anterolateral dislocations of the radial head, this relation becomes particularly intimate, causing a paresis of the nerve. In adults, there is a more discrete organization of the proximal border of the superficial head of the supinator, forming the arcade of Frohse. This band is not as well defined in children and, therefore, may partially account for the lower incidence of permanent injury to the posterior interosseous nerve, as well as the high incidence of resolution once the reduction of the radius is obtained.
The ulnar nerve is relatively tethered by the cubital tunnel and can be at risk in Monteggia fractures involving the proximal end of the ulna, particularly type II injuries.
Nonoperative treatment should generally involve three steps: correct the ulnar deformity, provide a stable reduction of the radial head, and relieve the deforming muscle forces, preventing recurrent radial head dislocation and ulnar angulation.
The first step is to reestablish the length of the ulna by longitudinal traction and manual correction of any angular deformities present. The forearm is held in relaxed supination as longitudinal traction is applied, with manual pressure directed over the apex until the angular deformity is corrected clinically and radiographically. With greenstick fractures, the plastic deformity must be corrected or the fracture completed to prevent recurrence of the angular deformity and/or re-dislocation of the radial head. Up to 10° of angulation is acceptable in a complete fracture, providing a concentric radial head reduction is maintained.
Once ulnar length and alignment have been reestablished, the radial head can be located. This is often accomplished simply by flexing the elbow to 90° or above, thus producing spontaneous reduction. Occasionally, posteriorly directed pressure over the anterior aspect of the radial head is necessary to facilitate reduction. Once the radial head position is thought to be established, it should be scrutinized radiographically in numerous views to ensure a concentric reduction.
Flexion of the elbow to between 110 and 120° stabilizes the reduction of the radial head by alleviating the force of the biceps, which could redislocate the radial head. The forearm is placed in a position of midsupination to neutral rotation to alleviate the forces of the supinator muscle and the anconeus, as well as the forearm flexors, which tend to produce radial angulation of the ulna.
Once the fracture is reduced and the neutral position is established, an above elbow cast or sugar tong splint can be applied. The plaster should be molded using three contact points to prevent recurrent angulation of the ulna. Once the cast is completed, careful radiographic assessment should be performed, and necessary changes made.
The patient is followed at 7- to 10-day intervals to confirm continued satisfactory reduction by radiography. At 3 to 4 weeks after the initial reduction, the above elbow cast is changed to a below elbow cast to allow early range of motion of the forearm, particularly pronation and supination. Full activity is allowed at 6 to 8 weeks after injury.
Although uncommon, there are two indications for operative treatment of the Monteggia fracture dislocation: failure of ulnar reduction and failure to reduce the radial head.
Galeazzi Fracture Dislocations
Although rare in children, another commonly pimped eponym is that of the Galeazzi fracture. Riccardo Galeazzi from Milan first described fractures of the distal radius associated with disruption of the distal radioulnar joint (DRUJ) in 1934.
In the uninjured wrist, little motion of the ulna occurs at the DRUJ due to the stabilizing forces of the ulnar collateral ligament, the volar and dorsal radiocarpal ligaments, the pronator quadratus muscle, the triangular fibrocartilage, and the dorsal and volar distal radioulnar ligaments. The exact mechanism that produces injury to these stabilizing structures is not well defined. It is established, however, that extremes of rotation and axial loading can contribute. Typically, the ulna will be dorsally displaced.
In two major reports that address treatment in children, investigators achieved good results in 90% of injuries treated by closed reduction alone. This is quite different from the adult counterpart of this injury, which is known as the “fracture of necessity,” meaning that operative intervention is a must. For Galeazzi fractures with a dorsally displaced ulna, there seems to be agreement that the optimal position of immobilization is with the forearm in supination. With the less common volar displacement, however, there have been reports of successful treatment in both supination and pronation.
The three major indications for operative management are instability with secondary proximal migration of the distal radial fracture fragment, inability to reduce the DRUJ due to interposed tendons, and inability to reduce the distal ulnar physis.
Hand and Wrist Injuries
Distal Radius Fractures
The distal forearm deserves special emphasis when discussing fractures in children because it is the most common area to sustain a fracture in the immature skeleton. As well, in many series, the distal radial physis is the most common pediatric physeal injury.
Compared to the adult, distal radial fractures in children are rarely intra-articular. Radial collapse, loss of wrist motion, and distal radioulnar joint dysfunction—all common problems associated with distal radial fractures in the adult—are rare after pediatric distal radius fractures. The incidence of complications and poor results is also relatively low in children. In one series of 1346 fractures of the forearm, only 7% required remanipulation. In another series of 1767 fractures, only 2.5% had any significant residual angulation. The distal radius has enormous remodeling potential due to the fact that 70-80% of forearm growth occurs distally. This may account for this low rate of unacceptable results.
The usual cause of a distal forearm fracture is the patient’s attempt to break a fall with an outstretched hand. Usually the wrist is dorsiflexed, which transfers the bending force to the distal radius. With this mechanism, the distal fragment is usually displaced dorsally.
In a physeal injury, the periosteum is usually intact on the same side to which the epiphyseal fragment is displaced (ie, compression side), and can be used to help stabilize the fracture after it is reduced. On the opposite, or tension side, the thicker periosteum remains attached to the perichondral ring and ruptures proximally in its thinner metaphyseal area. This wad of periosteum can become interposed in the fracture site and can subsequently interfere with the reduction.
Documentation of the neurovascular function is important in children’s distal radial metaphyseal and physeal injuries. Nerve injuries are most often neurapraxias of the median or ulnar nerve that result from stretch at the time of acute deformation, and only rarely is a major nerve trapped between the ends of the fractured bone. Nerve paralysis with a peculiar springy sensation noted during attempts to reduce the fracture may be the only indication of nerve entrapment within the fracture.
Closed reduction is usually easy unless the ulna is intact and the radius is completely displaced. Overreduction is rarely a problem because of the intact dorsal periosteum. Repeat manipulation of distal radial physeal injuries is not recommended because of the increased risk of growth disturbance. If the patient presents for treatment later than 3 days after the injury, primary manipulation of the fracture is not advisable, as forceful attempts are likely to damage the physis and result in growth arrest. General anesthesia may be required to provide adequate sedation in the event that late reduction must be performed.
Because the results with nonoperative management are so good, there are primarily only five specific indications for operative intervention: the need for percutaneous pin fixation because of severe local soft-tissue injury or proximal ipsilateral fractures; failure to achieve an adequate reduction by closed methods; open fractures; comminuted intra-epiphyseal fractures; and carpal tunnel compression or compartment syndrome
If severe soft-tissue injury accompanies the bony injury, as with a crushing injury or superficial abrasions, rigid external immobilization with a cast may not be adequate and could even compromise the circulation. In these cases, the surgeon can stabilize the fracture with a single pin placed percutaneously across the fracture site. Once the distal fragment is internally stabilized, the surgeon can place a loose-fitting cast, mainly for protection. The most common use for percutaneous pins is with ipsilateral supracondylar humeral fractures
A prompt reduction under adequate relaxation is important in the closed management of these fractures. If a significant delay in reduction occurs, a fibrous clot usually develops at the fracture site and may decrease the ease of reduction; the fracture may require a more forceful manipulation to obtain an adequate reduction. The more force applied across the fracture site, the greater the chance of injuring the proliferating cells of the physis; therefore, one should try to obtain a prompt reduction as gently as possible. During reduction, the surgeon should maintain traction across the fracture site to separate the fracture fragments and, theoretically, to decrease the shear forces on the physis with manipulation. The use of finger-traps with counter traction applied across the anterior portion of the flexed elbow can assist in maintaining traction during reduction. With traction applied, the surgeon can often easily reduce the fracture by simply pushing the distal fragment anteriorly and distally with the thumb
Immobilization for 4 weeks is typically adequate. Use of a volar splint for another 10 to 14 days provides comfort and protection from reinjury until the forearm muscle strength and wrist motion have begun to return to prefracture status.
Diligent follow-up is essential. X-rays at 4 to 6 months after the injury can help to ensure that normal growth has resumed. Symmetric migration proximally of the Harris-Park growth lines is a manifestation of normal growth. All fractures should be followed, because even the most benign-appearing ones may result in growth arrest.
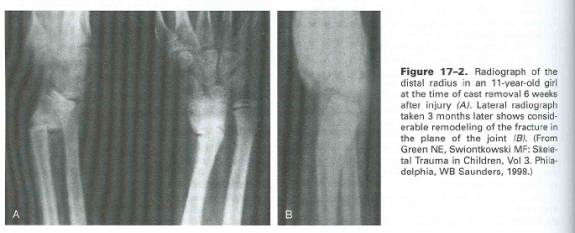
Distal radial physeal fractures are usually Salter-Harris type II Injuries, and can be treated similarly to distal radial metaphyseal injuries. It is important, however, to stress to the parents the increased likelihood of physeal growth arrest, and follow these injuries appropriately so as to catch any growth arrest as early as possible.
The two factors most directly related to this growth arrest are, the energy of the initial trauma, and iatrogenic injury with late reduction. To avoid being part of the problem, rather than the solution to it, one should avoid repeat reduction (closed or open) after 7 days from the time of the injury. If necessary, dorsal (as usually the deformity is apex volar) opening wedge osteotomy can be performed in the skeletally mature patient to alleviate the complications of malunion.
Hand
Several factors combine to make the pediatric hand vulnerable to injury. Among these are the usage pattern of this relatively exposed appendage and the child’s curiosity about the surrounding world. It should therefore come as no surprise that injuries of the hand and wrist are among the most common in the skeletally immature population.
The prevalence of these injuries increases sharply after the eighth year. This may be due to the changing balance between injury-resistant cartilage and bone in the maturing hand, and the fact that children participate more aggressively in contact sports around this age.
There is disagreement about which is the most common fracture in the child’s hand. Some authors cite the distal phalanx crush injury as the most frequent, others recognize the Salter-Harris (S-H) II fracture of the proximal phalanx base. Fractures of the phalanges outnumber metacarpal fractures. The right and left hands are equally affected by skeletal trauma. The border digits (the index and small fingers) are usually the most commonly injured rays. More boys than girls present with hand fractures.
Hand injuries involving the growth plate are less common than extraphyseal fractures, and reports vary between 10% and 40% in the reported series. Salter Harris II fractures predominate in all reports.
Most metacarpal and phalangeal injuries of the pediatric hand are non-displaced, and can be treated non-operatively. It is very important to respect the hand’s propensity for stiffening up in the position in which it is immobilized. Hand injuries should always be splinted in a position of function to protect against re-injury and debilitating stiffness often found when fingers are immobilized in a fully extended position. One of my earliest mentors used to say that the finger immobilized in extension on a tongue depressor is only good for one thing, “so the kid could point straight at you in court and say, ‘that’s the jerk who did this to me.’”

